How do you Ensure Healthcare Equity in Keeping with Your Institution’s Diversity and Inclusion Goals? It Takes a Systemic Approach
Aug 24, 2021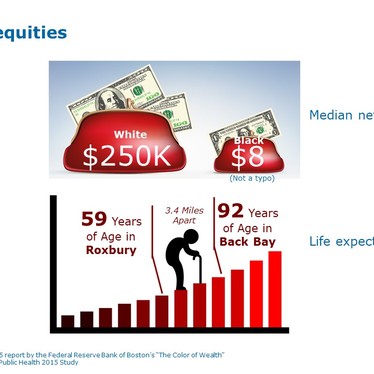
BY CYNTHIA MCGRATH | August 9, 2021
Racial justice protests and the disproportionate impact of COVID-19 on communities of color have shone a light on the need for organizations to improve diversity, equity, and inclusion (DE&I). The higher education industry has taken a leading role in tackling these challenges by evaluating and implementing policies that seek to ensure that all residents – regardless of gender, race, ethnicity, gender identity, or sexual orientation – have the same opportunity to thrive. Recent New England Journal of Higher Education and Higher Education Today editorials have encouraged colleges and universities to act now to eradicate disparities and promote economic vitality.
Numerous studies have shown that gender, race, and ethnicity have a marked influence on a person’s health. The systemic disparities in the health status of population groups have significant social and economic costs to people and societies. COVID-19 has exacerbated these differences in health outcomes and access to care. A 2015 Boston University of Public Health Study found a 33-year life expectancy gap between Boston’s Roxbury, a majority-minority community, and Boston’s Back Bay, a primarily white area. These communities are only 3.4 miles apart.
COVID-19 has only exacerbated these disparities and Hispanics and Blacks were the hardest hit. Life expectancy for Black residents decreased 2.1 years and 3.05 years for Hispanic residents, according to the Department of Public Health.
“The pandemic caused a perfect storm,” said Juan Lopera, inaugural Chief Diversity, Equity, and Inclusion Officer of Beth Israel Lahey Health. “Forty percent of Latinos work in the service industries and couldn’t work from home. They were scared to access care in part because of the policies of the previous administration. Black and brown people also have a higher prevalence of asthma and diabetes, so were at high risk for COVID-19 complications.”

Use a Systemic Approach to Achieve DE&I Objectives
How can we advance our educational institution’s DE&I objectives — especially through our employee healthcare benefit program? “To address inequities, it requires a systems approach,” said Juan Lopera. He recommends three strategies for making progress on Diversity, Equity, and Inclusion:
- Start the conversation: Conduct active listening sessions with your employees, students, and other stakeholders to find out their experiences. This will help inform your organization’s plan.
- Create a governance structure: Identify who will serve on your Diversity Task Force to take the learnings from your outreach and put plans into actions.
- Put together a five-year plan: Identify your organization’s goals, how you will measure progress toward each goal, and which items are priorities.
Tips for Identifying and Addressing Access Gaps
One Size Doesn’t Fit All – Use a Multi-pronged Approach
Determine roadblocks for minority access to goods and services and develop innovative approaches to reach all your constituent. “There is no equity in population averages,” said Mr. Lopera. He cited rates of COVID-19 vaccinations as an example of this phenomena. “Although Massachusetts is faring well in administering the vaccines, racial minorities are well below the average.”
He suggests that employers partner with community organizations to support vaccine equity. He helped spearhead such an operation when he was Vice President of Business Diversity for the combined Tufts Health Plan and Harvard Pilgrim Health Care organization (which will be known as Point32Health). Tufts and Harvard Pilgrim contracted with minority-owned businesses to bring the vaccine to the minority community in mobile vans.

Tackle Healthcare Data Collection Needs
There’s room for improvement in gathering race and ethnicity data for commercial health payers needed to analyze health disparities, utilization, costs, and opportunities for improvement. Only 3%-4% of commercial health plan data capture this information compared with approximately 80% for Medicare and Medicaid.
If your HR system isn’t collecting this data and sending it to the health administrator, determine how you can fix it, and work around it in the short term. “Don’t let the perfect be the enemy of the good,” said Mr. Lopera. “There’s options to supplement what you have with predictive data based on zip code and surname.”
How is your organization supporting gender equity and identity? Many of the legacy health data systems don’t have the flexibility for gender and gender identity indications needed for optimizing service and care coordination: gender at birth; gender identity; and sexual orientation.
Address Provider Network Holes
The recent widespread adoption of telehealth brings many new opportunities especially for behavioral health and substance use disorder needs. However, research among early users shows that certain groups are underrepresented, including non-English speaking patients, and patients of Asian, Black, and Latinx descent. Preventive care visits are similarly low – and use of emergency rooms is high – for minority populations in part due to culture and language barriers with healthcare providers. Mr. Lopera recommends that healthcare purchasers work with plan administers to identify and work to close ethnic and language gaps in your provider networks.
Other Insights
- Seek Out Diverse Vendors: Contracting with minority-owned businesses helps to address significant wealth inequalities impacting communities of color.
- Evaluate Your Endowment Investments: Is your educational institution investing its endowment funds in keeping with your diversity, equity, and inclusion goals? Your approach to investing speaks volumes about your commitment to DE&I.
- Improve Workforce Equity: increase rates of diversity in your workforce across all levels, particularly leadership. Commit to address racism in hiring and other policies.
Juan Lopera spoke at edHEALTH’s May 26, 2021 Thought Leadership Seminar. As Beth Israel Lahey Health’s new Chief Diversity, Equity, and Inclusion Officer, he leads and accelerates the health system’s efforts to transform care delivery for the underserved, while establishing diversity, equity, and inclusion capabilities. Prior to this position, he was Vice President of Business Diversity for the combined Tufts Health Plan and Harvard Pilgrim Health Care organization (Point32Health) and oversaw company-wide diversity efforts including health equity, multicultural customer offerings, supplier inclusion, and workforce equity and inclusion. He serves on several boards including as Vice-Chair of the Dimock Center Board, Co-Chair of The Boston Foundation’s Latino Legacy Fund, member of the State of Massachusetts COVID-19 advisory groups for health equity and vaccine communications, and member of the State's Latino Advisory Commission.


